Skills Corner - Are you smarter than a BVM?
Disclaimer: This is my opinion and does not reflect the view of any entity that I trade time for cash with. Everything is meant for educational food for thought and you should always “follow your protocols.”
Well, of course, you are, but I wanted to share some things that sparked my interest and highlight the not easy skill of ventilation.
First thing, first..... Bagging is a perishable skill!
You need to practice it at least once in a bit to build that mental model and recall ways to troubleshoot issues. Or as the AHA puts it, “bag-mask ventilation is a challenging skill that requires considerable practice for competency” Variables such as poor muscle tone, trauma, facial hair, lack of teeth, and that BVM that hasn't been touched in years.
What can we do or teach others about this and improve ventilatory compliance?
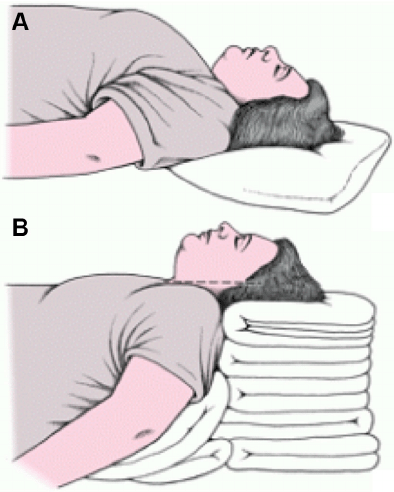
We need to start off with positioning the patient for success. Either ear to sternal notch for non-trauma patients or jaw-thrust for the cervical-impaired patient. This moves the tongue off the airway and makes the trachea the path of least resistance. For our infants, placing that towel under the shoulders prevents hyperflexion of the neck due to the proportionally larger head.
This is a good reason to keep those blankets stocked.
Ever heard of the smoking dragon? This is where you place 2 NPAs and an OPAs for maximum pharyngeal compliance. Does your airway bag have the required sizes to do this?
Now that we are ready to rumble, we need to get a great mask seal. If you are forced to bag all by yourself, the E-C clamp you learn in CPR is ok for a seal, but it is one-sided and you have to be on your game with that grip strength. The preferred method is a 2-person BVM with a 2-thumbs approach or to a lesser extent a double E-C clamp. This will maximize the surface area in that pressure is applied. This works well in CPR as this lets the compressor provide ventilation and keep rhythm with the cycle. For premature newborns, turn the mask upside down to keep oxygen from contacting the eyes. This can cause vasoconstriction of the vessels and has the chance to cause blindness or increased mortality.
NAEMSP Statement on Ventilation Management
Next, we are off to volume. The average tidal volume for IBW in males and females is about 400-500ish. Hence why we went to pediatric BVM's in cardiac arrest. Hyperventilation kills when you have too much oxygen which then causes vasoconstriction, more importantly, cerebral vasoconstriction. It's great to get the code save, only to deliver a vegetable to market, is not a true code save. Here is a picture of 500mLs of volume.
Image by www.FOAMFrat.com
“What 500mL looks like.” Image by www.FOAMFrat.com
That's how much you need to squeeze the bag. Why the adult is 1500-1600mLs of volume would be a great question. Even a 220lb person at the end range of 8mLs/kg which is still under a liter. If you use a BVM on a non-cardiac arrest. Just be aware of how much you are actually giving to the patient.
Moving on, we have the rate. Depending on your age and disease, you could have any number of ventilation rates. Just know what that is and stick to it. If you need to use the CareVent for hands-free bagging, then most definitely do it. Whether hyperventilating in head trauma or hypoventilation in cardiac arrest, know why you're doing it and keep an eye on that ETCO2.
With all of these things working in sync, you should have a perfectly ventilated and oxygenated patient. What if... things don't go as planned. You need to have a couple of options to try to troubleshoot your bagging.
Ramp obese patients and children to improve functional residual capacity
Try a smaller mask
Switch to 2-person
Move the mask off the chin to remove the valley under the mouth.
Or if you have not done any of the other items mentioned previously.
All done? Well, not just yet. I have one more thing to mention. You probably have seen it on your rescue, it has a red top and screws down from 5 to maybe about 20cmH2O. If you guessed the PEEP valve, then you are right. This device is soooo important, they should have them already added to the BVM. Just like with the yellow brick, we call a CPAP machine, it provides positive pressure to keep those alveoli open and allow for oxygen exchange. The great thing about this device is that it is almost plug-and-play. Just set it to 5cmH2O and go. You could turn the PEEP up more to allow for more expansion, but that's something I can't officially recommend due to the protocol. Generally, 5-8 is physiological PEEP and over 10cmH20 you start wandering into decreased perfusion territory depending on your patient.
For infants, this might be needed to push fluid from birth out of the lungs. See the Neonate resuscitation program for an algorithm for reference. COPD patients are prime candidates for PEEP, as that's the main reason why we use CPAP.
If you have to intubate for some reason, then make sure you continue that PEEP when ventilating. Upon transfer, you need to worry about clamping that tube for transfer to the hospital ventilator. If you don’t, you’ll lose that PEEP and it may be harder to get that expansion back, causing worse outcomes and/or arrest.